
Americans do not do end-of-life care well. As Atul Gawande explained in his most recent book, far too many terminally ill Americans spend their final days in the hospital undergoing painful and largely futile medical procedures, rather than in a potentially more comfortable home or hospice setting. This has a negative effect not only on the person who is dying him- or herself, but also on their friends and family — for one thing, as a team led by Dr. Amol Narang of the John Hopkins School of Medicine explains in a new article in JAMA Oncology, “hospital deaths are associated with worse mental health outcomes in bereaved caregivers.”
The culprit here is a lack of planning, particularly when it comes to (usually) slowly developing diseases like cancer. End-of-life (EOL) care is a difficult thing to talk about, and the transition from active medical treatment to palliative care entails the rather formidable psychological barrier of acknowledging that you’re “giving up” on saving the life of a loved one. At the same time, there’s a growing awareness that it’s important to have these discussions, and many health systems are experimenting with new ways to promote communication between patients, doctors, and loved ones about advance care planning.
Narang and his colleagues wanted to know whether Americans are making progress when it comes to EOL care, so they took a big, nationally representative survey known as the Health and Retirement Study (HRS), and examined data collected from the next-of-kin of Americans who died of cancer between 2000 and 2012, and interviewed them.
The authors were looking for trend lines: Have Americans, over time, become more likely to do the things that lead to a “good” death? That is, have they become more likely to get EOL preferences into writing, or to assign durable power of attorney to a friend or relative? Related, have they become less likely to die in a hospital, or more likely to turn down unnecessary, potentially pain-increasing medical care?
The overall answer, as these two charts from the study show, is that no, Americans aren’t getting better at most of this stuff:
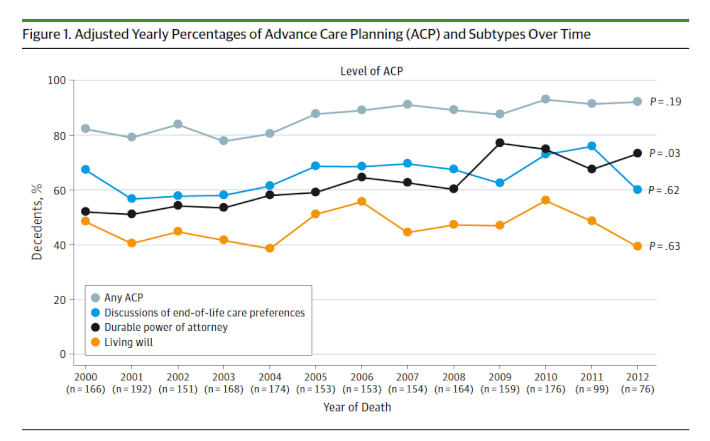
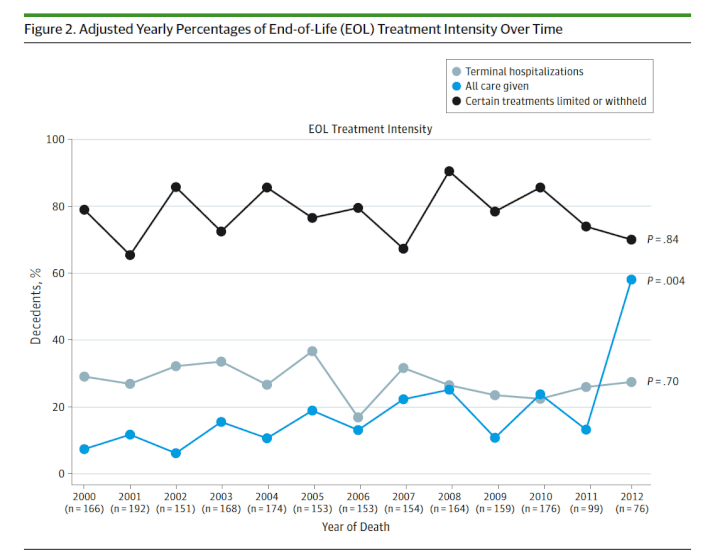
As you can see, the trend lines are mostly flat, which means that growing awareness of the problems with EOL care in the U.S. hasn’t been met with much action — at least not yet (statistically speaking, actual movement on the graph, rather than somewhat random bouncing around, would have a so-called p-value of less than .05).
That doesn’t mean this is a hopeless cause, of course: The authors cite the success story of La Crosse, Wisconsin (also highlighted in a fascinating “Planet Money” episode), which has achieved a high rate of EOL-care planning “through general awareness campaigns that promote [advance care planning] and an electronic record system that prompts all patients reaching age 55 years to discuss their EOL care preferences with their primary care provider, among other initiative.” And as Science of Us reported back in February, two hospitals in greater Boston got some very promising results simply by showing patients who were likely close to death a short video about some of the complications that can arise when patients at the end of life are given CPR or intubated.
So there are ways to improve EOL care in the U.S., at least based on these early results. But if this article is any indication, they just haven’t fully caught on yet.




